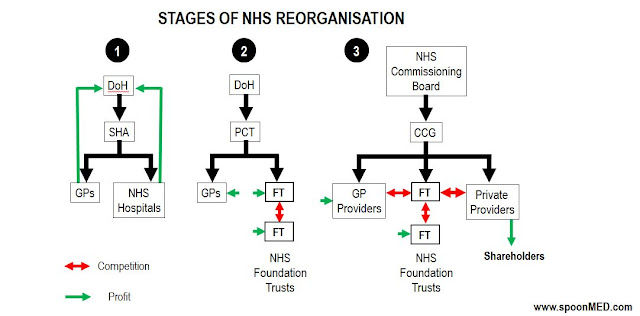
The Health and Social Care (HSC) Act
was passed in March 2012 and came into effect on April 1st 2013. GP
led CCGs (Clinical Commissioning Groups) became responsible for the NHS budget
and are now compelled to use competition as a means of improving NHS
services. To most of us this seems like a good thing at first glance. Many of
us are unaware of what this really means. To help public awareness, here is my
‘Elevator Pitch’ on NHS reforms. An Elevator Pitch is a summary of a concept or
argument, short enough to be delivered between floors in an elevator. In the
UK, we might call this a Lift Pitch.
The NHS is one of the most efficient
healthcare systems in the world. It provides universal, comprehensive
healthcare to EVERYONE. Healthcare is free at the point of delivery. We do not
run the risk of personal bankruptcy when we fall ill. NHS hospitals are run on
a non-profit basis where savings are reinvested in healthcare. Clinical
outcomes are excellent. The US spends 2.4 times more on health per person than the UK, yet
Britons live longer than Americans. Despite these achievements, the NHS has
come under significant attack in the media. Budget cuts at a time when the NHS
is at its most efficient have led to staffing shortages and ultimately problems
outlined in the Francis Report.
The HSC Act 2012 removes the Secretary of State’s legal obligation
to provide or secure healthcare for everyone. The NHS is also now subject to EU
Competition law. Section 75 (being debated in the House of Lords today) compels CCGs to invite bids for all health services
from ALL willing providers. This leads to a free
market based system where expensive tendering processes will consume much of
the CCG budgets and time. In the US, administration costs account for
20% of healthcare expenses, three times higher than in the UK.
Healthcare providers will compete against each other for the
contracts. This may improve some services. However, barriers between primary
care and hospitals will move us away from integration and data sharing. There
is a risk that profit making organisations will cherry pick lucrative
contracts, leaving difficult and expensive services to non-profit
organisations. The irony
is that a last minute amendment to the HSC Act makes this even more likely. The amendment declares that the only services NOT subject to competition law are those which can ONLY be provided by a current provider (most likely to be complex, expensive services).
As NHS budgets become tighter and
healthcare becomes more expensive (largely as a result of spiraling
administrative costs), the NHS is likely to change from a mostly single payer
(government funded) system to a US style multiple payer healthcare system, what Don Berwick refers to as a
‘zoo of payment streams’. We only have to look to the US to see how our
healthcare system might look in a few years.
Vinod Achan
For my blog on Don Berwick, see here.
Vinod Achan
For my blog on Don Berwick, see here.